Organisms grow by making more cells through division, then shaping those cells into specialized tissues through a process called differentiation. To understand how living things grow, it helps to look at cell division, differentiation, and the signals that control when and where growth happens how do living things grow class 3. They repair themselves using many of the same tools: stem cells divide to replace damaged ones, signaling molecules coordinate the response, and dedicated molecular machinery fixes errors in DNA before they become permanent. The whole system is tightly regulated, built-in feedback keeps growth from spiraling out of control, and when those controls fail, problems like cancer emerge.
How Do Organisms Grow and Repair Themselves? Core Biology
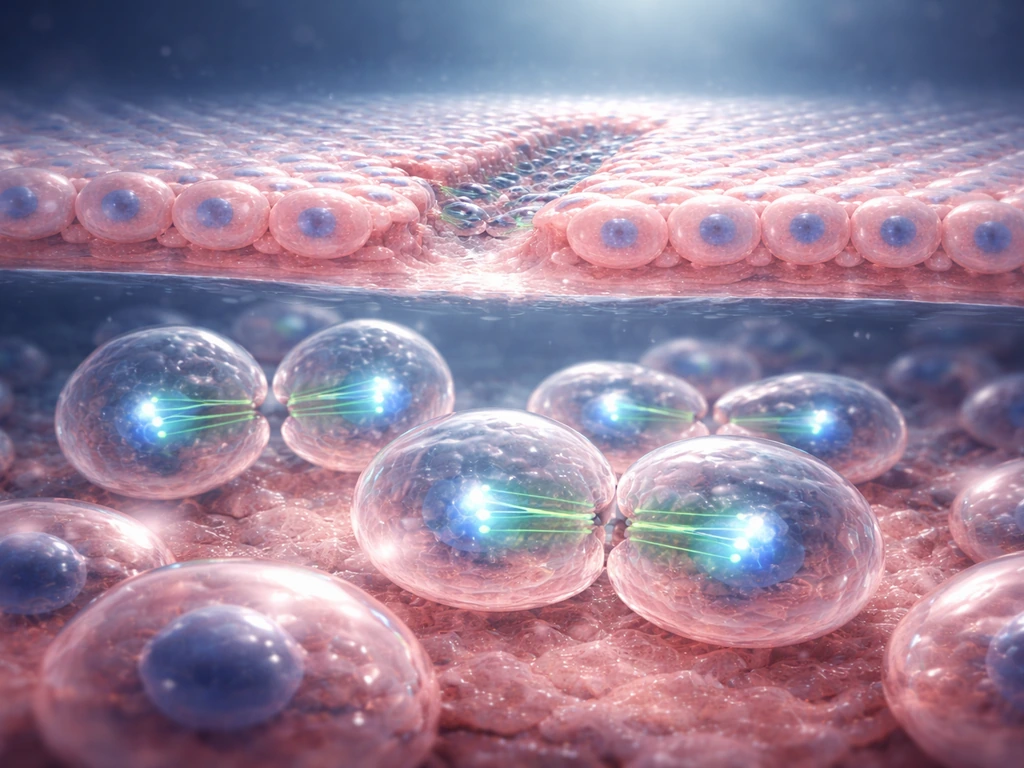
What 'growth' actually means in living systems

Growth in biology is not just getting bigger. It means increasing the number of cells, the size of individual cells, or the total amount of organized biological material (biomass) in a way that maintains function. A bacterium growing in a warm petri dish doubles its internal machinery and then splits in two. A human embryo starts as a single fertilized cell and, through trillions of coordinated divisions, builds a body with over 200 distinct cell types. Both are 'growing,' but the scale and complexity are radically different.
It helps to separate growth into two components: cell proliferation (more cells) and cell enlargement (bigger cells). Most tissue growth in animals is driven mainly by proliferation. Plants do both, and they also grow by expanding existing cells with water pressure inside rigid cell walls. Single-celled organisms like bacteria or yeast grow primarily by enlarging until they hit a size limit, then dividing. The common thread across all of these is that growth requires energy, raw materials, and coordination.
How cells divide and differentiate to build an organism
The cell cycle: your body's built-in copy machine
Every time a cell divides, it runs through a carefully staged cycle. Interphase is the long prep phase, split into G1 (cell grows and checks conditions), S phase (DNA is copied), and G2 (more growth, final checks). Then comes M phase, where mitosis divides the nucleus and cytokinesis divides the rest of the cell. Cytokinesis works by assembling a contractile ring of actin filaments that pinches the cell in two, like tightening a drawstring on a bag. The result: two daughter cells, each with a complete copy of the genome.
Growth factor signaling doesn't just tell a cell to divide. It simultaneously ramps up the cell's entire biosynthetic capacity, boosting protein synthesis, RNA production, lipid manufacturing, and energy output. Think of it like a factory getting a production order: the order triggers more workers, more machines, and more raw material deliveries, not just a press of one button. Division without matched biosynthesis would produce progressively tinier, useless cells.
From a blob of cells to a body: differentiation and tissue formation
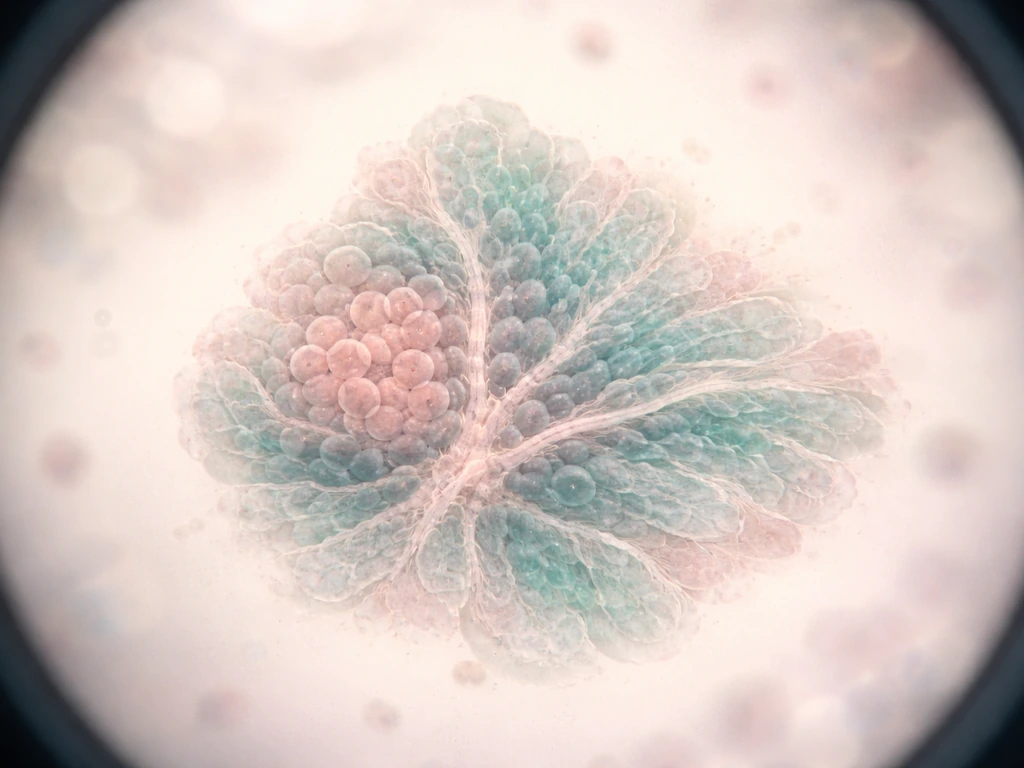
After cells divide, they don't all stay identical. Differentiation is the process by which cells read chemical signals in their environment and switch on specific sets of genes, committing to becoming a muscle cell, a neuron, a skin cell, and so on. Early in development, large-scale tissue movements like gastrulation physically relocate cells into new neighborhoods, exposing them to different signals and locking in new identities. One group of cells ends up near a signaling source; another group ends up far away. That difference in position translates directly into a difference in cell fate.
The signals that establish these positions are called morphogens. Sonic Hedgehog (Shh) and Wnt/BMP, for example, form opposing gradients across developing tissues, creating a positional coordinate system. Cells read their position in the gradient and express different genes accordingly, much like different neighborhoods on a map having different zoning rules. This is how a structurally complex limb or brain region gets built from what started as a uniform ball of cells.
How organisms regulate when and where growth happens
Left unchecked, cell division would be catastrophic. The body uses layered feedback systems to make sure growth happens in the right place, at the right time, and stops when it should. Morphogen pathways have built-in brakes: Shh signaling, for instance, triggers the production of Patched1 (Ptch1), an inhibitory receptor that dampens further Shh response. BMP signaling induces inhibitory Smad proteins (SMAD6 and SMAD7) that block its own output. These negative feedback loops act like a thermostat, preventing runaway signaling.
Wnt signaling uses a similar strategy. Proteins like Dickkopf (Dkk) and SOST act as inhibitors that compete with Wnt for binding to co-receptors like LRP5/6, damping excessive signaling. The result is a gradient with a precise shape rather than an unconstrained flood of signal. These feedback controls are not optional extras in development. They are baked into the pathway architecture itself, and mutations that disrupt them are a common route to developmental defects and tumors.
Growth regulation is also temporal. Different tissues have growth windows that open and close based on hormonal signals, nutrient availability, and developmental stage. Bone plates in humans fuse in late adolescence under hormonal influence, permanently ending length growth. Muscle tissue can still hypertrophy (enlarge existing cells) in adults, but the underlying regulatory logic is the same: signals open a growth window, feedback mechanisms close it.
What makes growth possible, and what limits it
Growth needs fuel and building blocks: glucose, amino acids, lipids, nucleotides, vitamins, minerals, and water. It also needs a stable internal environment, appropriate temperature and pH ranges that keep enzymes functional. Too far outside those ranges and the machinery slows or stops. This is why fever disrupts normal cell function, and why extreme cold halts the growth of organisms that can't regulate their own temperature.
Physics puts hard limits on how big a single cell can get. Oxygen diffuses into a cell from its surface, and the interior concentration drops the farther you go from the edge. For a spherical cell, the surface-to-volume ratio shrinks as radius increases (roughly 3/r for a sphere), meaning larger cells struggle to import enough nutrients and export enough waste relative to their needs. This is why the largest cells in your body are not spherical metabolic workhorses. They are either flat (like skin cells), highly branched (like neurons), or have specialized structures to increase surface area.
For multicellular organisms, circulatory and respiratory systems exist precisely because diffusion alone cannot supply oxygen and nutrients to deep tissues fast enough. Even in engineered tissue constructs grown in labs, cells more than a fraction of a millimeter from a nutrient source begin to die, which is one of the core challenges in regenerative medicine today. The bigger an organism gets, the more elaborate its delivery infrastructure needs to be.
How living things repair damage: wound healing and maintenance
When you cut your skin, your body launches a coordinated repair response that unfolds in four overlapping phases: haemostasis, inflammation, proliferation, and remodelling. Understanding these phases makes it clear that repair is not passive recovery but active reconstruction.
- Haemostasis: Within seconds to minutes, platelets detect exposed collagen at the wound site via integrin receptors and activate, triggering clotting to stop bleeding and seal the breach.
- Inflammation: Immune cells flood the site, clearing debris and pathogens while releasing signals that recruit repair cells. This phase is essential but destructive if it runs too long.
- Proliferation: Fibroblasts and other cells pour in to build granulation tissue, a temporary scaffold of fibronectin, collagen, and glycosaminoglycans packed with new blood vessels and immune cells.
- Remodelling: The temporary scaffold is replaced with organized collagen over weeks to months, restoring tensile strength. Scar tissue in humans is the result of this remodelling, which never quite recreates the original architecture.
Chronic wounds, like diabetic foot ulcers, are often stuck in the inflammatory or early proliferative phase, unable to progress to remodelling. Understanding that healing is a progression with regulatory checkpoints helps explain why some wounds heal cleanly and others do not.
Beyond acute injuries, most tissues are in a constant low-level maintenance mode. The lining of your gut replaces itself completely every few days. Red blood cells live about 120 days and are continuously replaced by stem cells in the bone marrow. Skin cells are shed and replenished constantly. This ongoing replacement is a form of repair, maintaining tissue function despite normal wear and tear.
Regeneration vs repair: why some organisms can regrow whole limbs
Humans repair; salamanders regenerate. That difference comes down to what happens at a cellular level after a major injury.
Planarians (flatworms) can be cut into many pieces and each piece will regrow into a complete animal. This works because they maintain a large population of adult stem cells called neoblasts distributed throughout the body. When amputation occurs, neoblasts show two distinct waves of increased mitotic activity within the first hours, ramping up to fuel regeneration. Within about half a day of the cut, a wound-response program is already active, with specific genes switching on, neoblast proliferation increasing, and apoptosis elevated near the wound to clear damaged cells and signal for replacement.
Salamanders use a different strategy. After a limb is amputated, the wound closes and a structure called a blastema forms, a mass of dedifferentiated progenitor cells. Skeletal muscle satellite cells are activated into a multipotent population that contributes to this blastema, effectively winding the developmental clock backward to rebuild what was lost. Macrophages from the immune system play a timed role: in zebrafish fin regeneration, for instance, macrophages accumulate mainly after blastema formation, suggesting they modulate rather than initiate the regenerative response.
Humans can do limited regeneration (liver regrowth after partial removal is the classic example), but most of our repair ends in scar tissue rather than perfect reconstruction. The reasons are still being actively researched, but leading factors include a more aggressive inflammatory response that forecloses the regenerative window, a less plastic pool of adult stem cells, and developmental programs that are more thoroughly locked down after embryogenesis.
| Feature | Planarians | Salamanders | Humans |
|---|---|---|---|
| Main repair cell type | Neoblasts (adult stem cells) | Blastema (dedifferentiated progenitors) | Tissue-specific stem cells + fibroblasts |
| Extent of regeneration | Whole body from a fragment | Full limb including bones and nerves | Partial (liver, skin surface); most tissues scar |
| Immune role in regeneration | Wound response, apoptosis near wound | Macrophages modulate after blastema forms | Strong inflammation, often limits regeneration |
| Speed of initial response | Gene expression within 0.5–12 hours | Blastema forms within days | Haemostasis within minutes; proliferation days later |
Cell repair and error control: DNA repair, checkpoints, and cancer risk
Every time a cell copies its DNA, errors happen. Your body makes billions of new cells every day, and each division copies about 3 billion base pairs. Even a very low error rate would be catastrophic without dedicated repair systems.
DNA repair mechanisms
Mismatch repair (MMR) is one of the primary proofreading systems. It scans newly replicated DNA for mismatched base pairs, excises the incorrect nucleotide, and fills in the correct one using DNA polymerase before sealing the strand with DNA ligase. Other pathways handle more severe damage: homologous recombination (HR) repairs double-strand breaks using the sister chromatid as a template, and non-homologous end joining (NHEJ) stitches broken ends back together when no template is available (though NHEJ is more error-prone). Defects in any of these pathways directly increase cancer risk by allowing mutations to accumulate and genomic instability to grow.
Cell-cycle checkpoints: the safety gates
Before a cell is allowed to divide, it must pass through a series of checkpoints. The G1 checkpoint checks whether conditions are right and DNA is undamaged. The G2 checkpoint confirms DNA replication was completed accurately. The spindle assembly checkpoint (SAC) at the end of mitosis prevents chromosome separation until every chromosome is properly attached to the spindle, preventing daughter cells from getting the wrong number of chromosomes.
p53 is the central enforcer of these checkpoints. When DNA damage is detected, p53 can halt the cell cycle to allow repair, or trigger apoptosis (programmed cell death) or senescence if the damage is too severe. Loss of functional p53 is found in a large proportion of human cancers because without it, damaged cells bypass the checkpoints and continue dividing, accumulating further mutations. Populations of cells with checkpoint defects tend to accumulate mutations far faster than normal because the occasional malfunction in replication, repair, or spindle assembly goes uncaught.
Cancer, in this framework, is not a mysterious external attack. It is what happens when the normal growth and repair machinery loses its error-control layers, allowing cells to grow without restraint. Understanding growth and repair mechanisms at this level makes it clear why cancer research so often focuses on cell-cycle regulation, DNA repair pathways, and checkpoint proteins.
Where to go next if you want to understand this more deeply
If this is clicking for you, the natural next step is to zoom in on mitosis itself and how it connects directly to how living things grow and repair. From there, exploring how plants and animals differ in their growth strategies gives a useful comparative view, since plants lack the mobile immune cells and circulating stem cells that animals use, relying instead on localized meristematic tissue. Thinking about what nutrients specifically support growth and how nutrient sensing ties into cell-cycle regulation is another productive thread.
For practical observation, you can watch wound healing directly on your own skin. A minor abrasion goes through all four phases in real time over a week or two, redness marking inflammation, the firm tissue of granulation, and the eventual flattening and fading of the scar during remodelling. Growing yeast cultures and observing exponential growth followed by plateau (as nutrients run out) is a classic and accessible experiment that makes the resource-limitation constraint viscerally real. If you want to go deeper conceptually, the keywords to chase are: morphogen gradients, cell-cycle checkpoints, stem cell niche, blastema formation, and contact inhibition (the mechanism that tells normal cells to stop dividing when they bump into neighbors, which tumor cells often lose).
Growth and repair are not separate systems with different logics. They are the same core toolkit, cell division, signaling, differentiation, and quality control, applied in different contexts. Getting comfortable with that idea unlocks a huge amount of biology.
FAQ
Do organisms repair by growing new cells, or by fixing the damaged ones?
Both. Many repairs use “same-cell” fixes, like DNA repair pathways that correct errors before division. Other repairs replace lost or irreversibly damaged cells through proliferation of stem or progenitor cells, then differentiation to restore the right tissue type.
Why can’t cells just keep dividing to fully repair tissue after an injury?
Repair needs the right timing and limits. If cells divide without proper biosynthesis, differentiation cues, and checkpoint control, tissue architecture fails. In many humans injuries, the regenerative window closes because inflammation and loss of plastic stem/progenitor capacity shift the outcome toward scarring.
What determines whether a wound heals with regeneration or with scar tissue?
A major factor is the balance between inflammation and regeneration signaling. When inflammation is prolonged or regenerative pathways cannot progress through to the later remodelling stage, the tissue reconstructs with collagen-rich scar instead of rebuilding the original structure and cell types.
How do cells know where to grow or repair, so they do not expand in the wrong place?
They use positional information and local feedback. Cells read morphogen gradients for identity cues and rely on inhibitors and “brakes” in signaling pathways. This is why disrupting gradient formation can cause abnormal patterning, even if cell division machinery is intact.
If morphogens form gradients, what prevents the gradient signal from becoming uniform everywhere?
Gradient shape depends on how signals are produced, spread, and actively inhibited. Negative feedback (for example, pathway-specific inhibitory proteins) helps prevent runaway signaling, and spatial differences in receptor availability or signal degradation maintain variation across tissues.
Why is fever disruptive to growth and repair?
Fever raises body temperature away from the optimal range where enzymes and protein folding work efficiently. That slows cellular processes, can worsen stress responses, and can interfere with the coordinated steps of wound healing and normal tissue maintenance.
What role do stem cell “niches” play in repair?
Stem cells are not only controlled by systemic signals, they also depend on local niche conditions like neighboring cell types, extracellular matrix, and concentration of growth factors. When niches are damaged or the niche signals shift, stem cells may stop proliferating or fail to produce the correct lineage during repair.
Can organisms repair damaged DNA and still divide normally?
Yes, if the damage is repaired within checkpoint time. Checkpoints can pause the cycle, giving repair systems time to fix lesions. If repair fails or damage is severe, cells may undergo senescence or apoptosis, which prevents propagation of mutations.
What is the most common mistake in understanding cell cycle checkpoints?
Thinking they only “detect” damage. In reality, checkpoints coordinate outcomes by halting progression, altering gene expression, and directing repair versus cell death. This decision-making is why checkpoint defects often lead to faster mutation accumulation and cancer risk.
Why do large animals need blood and breathing systems, but small ones can rely on diffusion?
Diffusion rates limit how far nutrients and oxygen can travel before cells lose adequate supply. Larger organisms require transport systems to deliver oxygen and substrates quickly to deep tissues, and diffusion alone becomes insufficient beyond short distances.
Why do yeast or bacteria grow fast at first, then slow down?
Their initial exponential growth depends on abundant nutrients and space. As resources deplete or waste accumulates, cells hit growth-limiting conditions, so they transition from rapid division to a slower growth or plateau state.
Is regeneration in salamanders completely different from human repair?
It uses some shared core ideas, like cell proliferation, signaling, and quality control, but the cellular strategy differs. Humans more often lack a widespread, highly plastic adult progenitor response, while salamanders form a blastema with dedifferentiated progenitors that rebuild lost structures.
Nutrients Which Help Us to Grow: What to Eat and Why
Protein, vitamins, minerals and calories explained for growth, plus meal tips and signs of low-growth nutrient gaps.


