Yes, scientists should be allowed to grow animals in artificial wombs, but only under strict, measurable, and independently enforced conditions. That's not a fence-sitting answer. It's the only position that takes both the biology and the ethics seriously at the same time. The science behind artificial womb research is genuinely promising, the welfare risks are real, and the difference between responsible use and reckless use comes down to whether the right safeguards are in place before the work begins, not after.
Should Scientists Be Allowed to Grow Animals in Artificial Wombs?
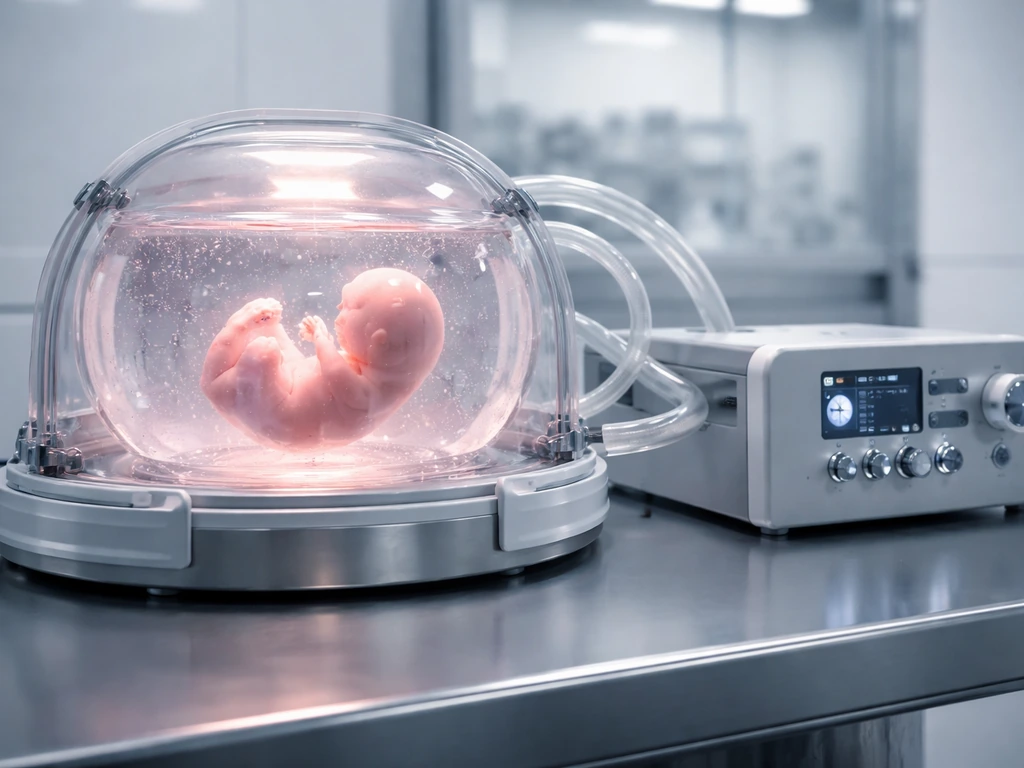
What artificial wombs are and what "growth" actually means here

An artificial womb, also called an ectogenesis device or artificial womb technology (AWT), is a controlled external environment designed to support the development of an embryo or fetus outside of a biological uterus. Think of it less like a science fiction tank and more like an extremely sophisticated life-support incubator. The goal is to replicate the biological conditions that a uterus provides so that a developing organism can continue to grow, differentiate, and mature.
"Growth" here means something more specific than just getting bigger. However, questions like can we grow organs add extra layers beyond ectogenesis itself. In developmental biology, growth involves three overlapping processes: cell proliferation (cells dividing through mitosis to increase in number), cell differentiation (cells becoming specialized tissue types like cardiac muscle, neural cells, or lung epithelium), and morphogenesis (those differentiated cells organizing themselves into functional organs and body structures). All three have to happen in the right sequence, at the right rate, and under the right conditions. Skip one, rush another, or get the chemistry wrong, and development doesn't just slow down, it can go wrong in ways that are hard to detect until it's too late.
So when researchers talk about "growing" an animal in an artificial womb, they're really asking: can we keep these tightly choreographed developmental programs running normally without a biological mother? This is also why organ-focused goals, like whether can scientists grow organs in lab systems, are adjacent considerations once you understand what “growth” requires for development. That's a much harder question than it looks.
How development can be supported outside the uterus
The uterus does a remarkable number of things simultaneously, and any artificial system has to match all of them at once. Here are the core biological requirements that an artificial womb must meet for development to proceed normally.
Oxygen and nutrient delivery

In a natural pregnancy, the placenta handles gas exchange and nutrient transfer. It delivers oxygen and glucose to the fetus and removes carbon dioxide and waste. Artificial systems replicate this with oxygenators and perfusion circuits, essentially pumping oxygenated fluid through a substitute for umbilical vessels. Getting the oxygen tension exactly right is critical: too little and cells die, too much and you generate toxic reactive oxygen species that damage developing tissue. Current research-grade systems use closed-loop monitoring to adjust this in real time.
Temperature and fluid environment
Cell division rates, enzyme activity, and protein folding are all temperature-sensitive. Most mammalian development happens at around 37°C (98.6°F), and even small deviations can alter the pace of mitosis or trigger stress responses. Beyond temperature, the fetus needs to be suspended in fluid, specifically amniotic fluid, which cushions it, maintains pressure, and contains growth factors, hormones, and antimicrobial compounds. Artificial systems have to approximate this composition closely, and researchers are still figuring out exactly what the full recipe should be.
Hormonal and biochemical signaling
Development is not just a mechanical process. It's driven by signaling molecules: hormones, growth factors, and cytokines that tell cells when to divide, when to stop, and what to become. A biological mother provides many of these through the placenta and amniotic fluid. Replicating this biochemical environment artificially is one of the hardest parts of the problem. Researchers are still mapping which signals are most critical at which developmental windows.
Waste removal

Metabolically active cells produce waste constantly. In a normal pregnancy, fetal kidneys filter waste into amniotic fluid, which is then recycled. Artificial systems need dialysis-like mechanisms to remove metabolic byproducts before they accumulate to toxic levels. This is one of the key engineering challenges that makes artificial womb systems expensive and technically demanding to operate.
Developmental milestones and monitoring
Normal development has measurable checkpoints: organ formation timelines, expected fetal movement patterns, lung maturation markers, brain development stages. Researchers can track these in artificial systems using ultrasound, biomarker sampling from the fluid, and continuous physiological monitoring. Deviations from expected milestones are the primary signal that something is going wrong, which is why monitoring is not optional, it's central to the entire enterprise.
What researchers could actually learn and improve
The scientific potential here is significant, and it's worth being specific rather than vague about it.
- Understanding developmental biology at a mechanistic level: researchers can isolate specific variables (oxygen, a particular growth factor, temperature fluctuations) in ways that are impossible to do inside a living mother. This kind of controlled experimentation is how we learn which conditions are truly necessary for normal cell differentiation versus which ones are just along for the ride.
- Improving outcomes for extremely preterm infants: current neonatal intensive care can support some premature infants, but the biological gap between a very early preterm and a full-term newborn is enormous. AWT research in animal models could lead to systems that bridge that gap more effectively.
- Reducing harm in some research contexts: certain developmental studies currently require pregnant animals to be present throughout an experiment. AWT systems could allow that research to proceed with fewer animals and with more controlled, reproducible conditions.
- Safety testing for drugs and environmental exposures: the fetal period is one of the most sensitive developmental windows for toxicant exposure. AWT systems could allow direct, controlled testing of how substances affect development at specific stages, without the confounding variables of maternal metabolism.
- Insights into growth constraints: questions like why cell growth slows at certain developmental stages, what limits organ size, and how growth programs are encoded, all connect directly to fundamental biology of cell division and physical constraints on development. This kind of knowledge has relevance far beyond AWT itself.
This is also directly relevant to related research questions in developmental biology, like whether stem cells can be used to grow organs in controlled environments, and how transplanted or lab-grown tissues establish normal growth patterns after placement. It also connects to questions like do transplanted organs grow after placement, since that kind of growth pattern is closely related to how tissues establish themselves in a new environment. AWT research generates foundational knowledge that feeds into those adjacent areas too.
Ethical risks and animal welfare concerns you can't ignore

The 2026 scoping review published in the Journal of Perinatology identified seven major categories of ethical concern around artificial womb technology: benefits versus harm, decision-making authority, moral and legal status of developing organisms, justice and access, cultural and societal perspectives, research ethics, and speculative concerns about future applications. That's a broad landscape, and not all of these concerns carry equal weight in an animal research context specifically, but several of them do.
Welfare risks from abnormal development
This is the most immediate and measurable concern. If the artificial environment does not perfectly replicate the biological conditions needed for normal growth, the developing animal may experience abnormal cell differentiation, organ malformation, or prolonged physiological stress. Unlike a healthy pregnancy, there's no biological feedback loop between mother and fetus that can make compensatory adjustments. The engineering has to be right from the start. A fetus that develops in a suboptimal artificial environment may suffer in ways that are difficult to detect in real time, which is an animal welfare problem that requires honest, upfront acknowledgment.
Moral status questions
A fetus developing in an artificial womb occupies a genuinely novel moral and legal position. It is not inside a mother whose welfare and rights are legally recognized. It is not a born animal with the protections that apply post-birth. Current animal research regulations were not written with this scenario in mind. The 2022 PubMed-indexed ethics review on AWT for the "fetonate" highlights exactly this gap: our ethical frameworks tend to have clear rules at the endpoints (the embryo, the born animal) but are much less clear about developing organisms in between.
Misuse and scope creep
Once the technical capability exists, it becomes harder to limit applications. Researchers working in good faith on welfare-improving applications could create infrastructure and knowledge that others repurpose for ethically problematic goals, such as growing animals to abnormal developmental stages purely for commercial purposes, or using the technology to justify removing legal protections for pregnant animals in other research contexts. Governance frameworks need to anticipate this, not just react to it.
Equity and regulatory fairness
If AWT research moves fast and produces clinical applications (especially if it eventually extends to human applications), access and fairness become real concerns. If your goal is to ask, “is it ethical to grow human organs,” the same welfare, governance, and misuse concerns apply, but the stakes and regulatory complexity rise sharply. Research conducted under well-resourced institutional conditions could generate technologies that are commercially deployed without equitable access, creating a situation where the scientific benefits are widely distributed in the literature but the practical benefits are not.
What governance should actually look like

The FDA has already begun developing guidance in this area. Their published documents on "Animal Study Considerations for Artificial Womb Technology Devices" and "Animal Study Design for AWT" represent a regulatory agency taking this seriously enough to produce structured planning frameworks for how animal studies should be designed and justified. That's a meaningful starting point, not a finish line.
A responsible governance framework for AWT animal research should include the following components.
- Independent ethical review before any study begins: not just institutional sign-off, but external review by a panel that includes developmental biologists, animal welfare experts, bioethicists, and a public representative. The FDA's animal study design guidance provides a framework, but review should go beyond device-safety questions to include welfare and scientific justification.
- Explicit developmental endpoint limits: studies should specify in advance how far along development will proceed in the artificial womb, and this limit should be set based on animal welfare considerations (specifically, the point at which the developing organism becomes capable of experiencing pain or distress). Research should not extend beyond that point without a separate and more rigorous approval process.
- Mandatory real-time welfare monitoring: continuous physiological monitoring tied to pre-specified intervention thresholds. If the fetus deviates from expected developmental milestones or shows signs of distress, there must be a pre-agreed response protocol, not a judgment call made under pressure.
- Transparent reporting of failures and negative results: the history of biomedical research is full of suppressed negative data. For AWT research specifically, failed experiments, abnormal developmental outcomes, and welfare incidents must be publicly reported. This is essential for building an accurate scientific picture of what the technology can and cannot do safely.
- Prohibited applications list: certain uses should be ruled out from the start. These include growing animals beyond the point of sentience for non-therapeutic purposes, commercial applications without separate regulatory approval, and any research whose primary goal is to circumvent existing animal welfare protections rather than advance genuine scientific understanding.
- Periodic re-review as the science evolves: governance frameworks written today will not anticipate everything. There should be scheduled reviews (at least every two to three years) where oversight committees assess whether current rules still match the state of the technology and the evidence on welfare outcomes.
When it's acceptable vs. when it's not: a practical decision guide
Not all AWT animal research proposals are equivalent. Here's a clear framework for evaluating whether a specific proposal sits on the acceptable side of the line.
| Criterion | Acceptable | Not Acceptable |
|---|---|---|
| Scientific justification | Clear hypothesis, knowledge gap identified, cannot be answered by less invasive means | Curiosity-driven, duplicative, or primary goal is technical demonstration rather than biological knowledge |
| Developmental endpoint | Limited to pre-sentience stage with biological justification for the chosen endpoint | Open-ended or extended to late-stage development without specific welfare review |
| Welfare monitoring | Continuous, with pre-specified intervention thresholds and humane endpoints | Periodic checks only, or thresholds left to researcher discretion at the time |
| Oversight | Independent external review plus institutional animal care committee approval | Internal approval only, no external ethical review |
| Reporting | Full public reporting of outcomes including failures and welfare incidents | Only positive results reported, or reporting delayed indefinitely |
| Application scope | Therapeutic research, developmental biology, welfare improvement | Commercial production, regulatory circumvention, or applications beyond the approved protocol |
| Animal selection | Species chosen based on biological relevance to the research question, with justification | Species chosen for convenience or to exploit regulatory gaps |
The biology matters here in a specific way. The question of when a developing animal becomes capable of experiencing pain and distress is not purely philosophical. It's tied to measurable developmental events: the formation of nociceptive neural pathways, cortical connectivity, and stress-hormone response systems. These happen at different gestational stages in different species, and setting welfare-based endpoint limits requires knowing those milestones for the specific animal being studied. That's a scientific question with a knowable answer, and it should drive the governance framework, not be an afterthought.
How to evaluate proposals and evidence today: your next steps
If you're a student, educator, researcher, or policymaker trying to evaluate a specific AWT research proposal or the field more generally, here's where to start.
- Read the FDA's published guidance documents on AWT animal studies. The "Animal Study Considerations for Artificial Womb Technology Devices" PDF and the companion animal study design document give you the current regulatory baseline in the US. They tell you what the agency considers a justified animal study and how such studies should be structured. This is the starting point for any regulatory evaluation.
- Look for the developmental milestone data in any research proposal or publication. Good AWT research will specify what stage of development the system supports, what the expected biological markers of normal development are, and how the team will detect deviations. If that information is absent, that's a red flag.
- Check for independent welfare oversight. Was the study reviewed by anyone outside the research institution? If not, treat its welfare claims with appropriate skepticism. Internal review alone is not sufficient for research in this area.
- Ask what the failure rate is and what happened when things went wrong. Published papers that report only successful developmental outcomes without describing failures or welfare incidents are not giving you the full picture. Search for the methods section details on humane endpoints and what happened when they were triggered.
- Consult the 2026 Journal of Perinatology scoping review on ethical considerations for AWT. It maps the full landscape of ethical debate across seven themes and gives you a structured way to categorize the arguments you'll encounter, whether they're about animal welfare, moral status, justice, or speculative future applications.
- Compare what's being claimed against what's biologically possible today. The science of organ development, cell differentiation, and developmental growth constraints has known limits. If a proposal or product claim implies that current AWT technology can support normal development in a way that hasn't been validated in peer-reviewed animal studies, be skeptical. The biology doesn't make exceptions for commercial timelines.
- Follow the transparency: does the institution or company conducting the research publish its protocols, its adverse event data, and its peer-reviewed results openly? Responsible AWT research should be generating public scientific knowledge, not proprietary techniques protected from scrutiny.
The bottom line is this: the question isn't whether artificial womb research on animals should happen at all. These same questions raise a broader issue: can we grow organs as well as animals in artificial wombs? You can even ask related questions like whether you can grow a brain in a lab, not just an embryo in an artificial womb can you grow a brain in a lab. Some of it is already happening, the FDA is writing guidance for it, and the scientific and medical case for doing some of it carefully is legitimate. That same “grow enough cells for research” challenge shows up in many lab settings even before any artificial-womb work begins. The real question is whether the specific research being proposed or funded meets a clear, biology-grounded, independently enforced standard for welfare and scientific rigor. That's a question you can actually answer, with the right information in hand.
FAQ
What counts as a “strict, measurable” welfare safeguard for animals in artificial wombs?
Not automatically. You should look for pre-registered welfare endpoints tied to species-specific developmental milestones (for example, when nociceptive pathways or stress-hormone response systems emerge), plus a plan for what happens if monitoring shows the fetus is outside expected ranges (early termination criteria, not just “adjust the device”).
If the device keeps the fetus alive, does that mean the experiment meets the ethical standard?
Researchers should distinguish between technical equivalence (the device keeps the animal alive) and developmental equivalence (the animal develops with expected organ maturation and stress profiles). A proposal that relies only on survival metrics, without milestone-based checkpoints and behavioral or physiological follow-up after removal, should be treated as insufficient.
How should governance address the risk of “too-late detection” of abnormal development?
A key edge case is whether the study can detect problems early enough to prevent serious harm. If the monitoring relies mainly on occasional sampling rather than continuous physiological signals, the system may miss fast-onset stressors or abnormal differentiation trajectories that worsen after a late intervention window.
What does “independently enforced” mean in practice for artificial womb experiments?
Independent enforcement should include both an external review component (ethics and regulatory oversight) and operational independence (audits of device logs, monitoring data, and adverse event reporting). Internal committees alone are not enough if they cannot verify real-time adherence to endpoints and stopping rules.
How should rules treat studies that go beyond welfare-improving goals, even if they are scientifically framed?
Yes, governance can require a “purpose limitation” test. For example, growing animals to abnormal developmental stages solely to expand commercial outputs should trigger a heightened review, even if the device is capable, because the welfare burden increases while the scientific justification may be weak or incremental.
What data should a responsible proposal collect to prove the device is improving welfare, not just running experiments?
Before approval, proposals should specify what will be measured to demonstrate that interventions improve outcomes, not just that they run successfully. This can include predefined organ maturation markers, waste-removal performance targets, oxygen tension ranges, and stress indicators, with a statistical plan for expected variability.
What safeguards should exist for device malfunctions or monitoring/calibration failures?
Prior to starting, teams should have a clear contingency plan for device failure, power interruptions, and equipment drift (calibration schedules). Because there is no biological feedback loop from a mother, ethics approvals should require rapid-response procedures and backup systems that are tested and logged.
Should ethical standards include follow-up after the animal is removed from the artificial womb?
Often, yes. For instance, post-exposure follow-up should include outcomes that might not be visible during the time in the device, such as longer-term growth, organ function, or persistent stress-related effects. A governance framework that stops at in-device milestones may miss significant harms.
How can committees avoid using vague ethical language that does not translate to measurable animal outcomes?
A common mistake is importing human-centered ethics debates without translating them into animal research endpoints. In animal studies, governance should emphasize species-appropriate definitions of distress and pain timing, and ensure that endpoint selection is grounded in biological knowledge rather than generic ethical language.
How can policy address misuse risk once the technology and methods become broadly available?
Researchers should plan for governance of downstream use, including restrictions on sharing device parameters or protocols that could enable misuse. Even well-intentioned platforms can lower barriers for repurposing, so policies for data sharing, IP controls, and access to device settings can be part of responsible governance.
Can Scientists Grow Organs in the Lab? What’s Possible Now
Can scientists grow organs now? Learn what organoids, bioprinting, and vascular limits enable and what still can’t.