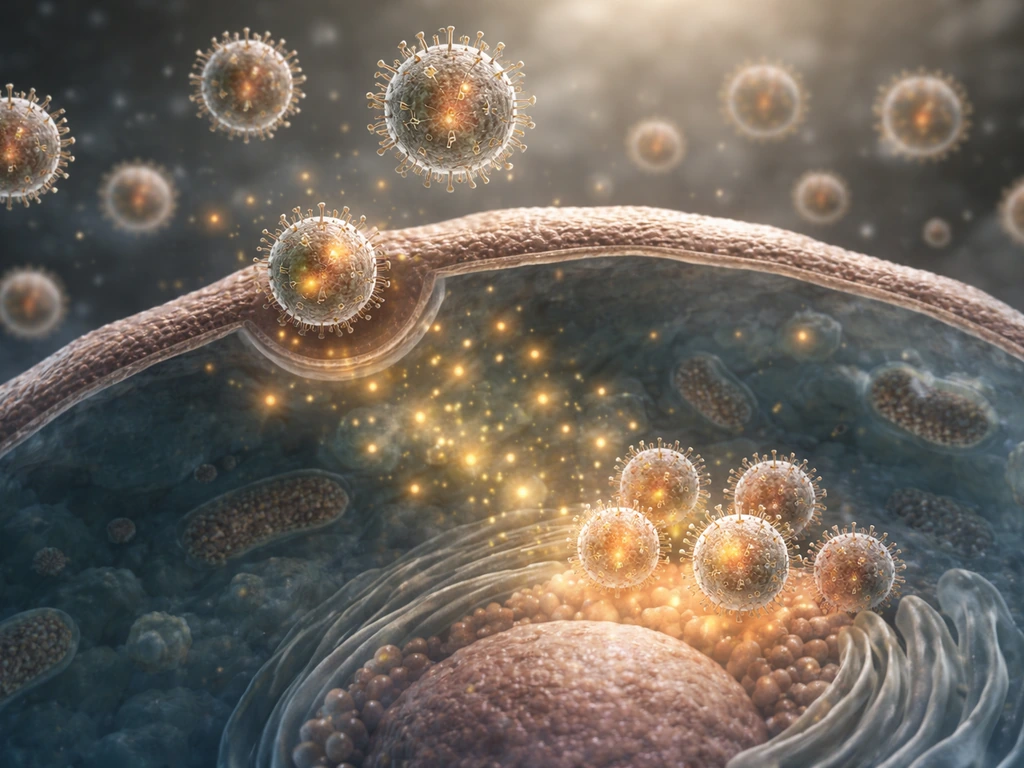
"Growth" vs. replication: what actually changes
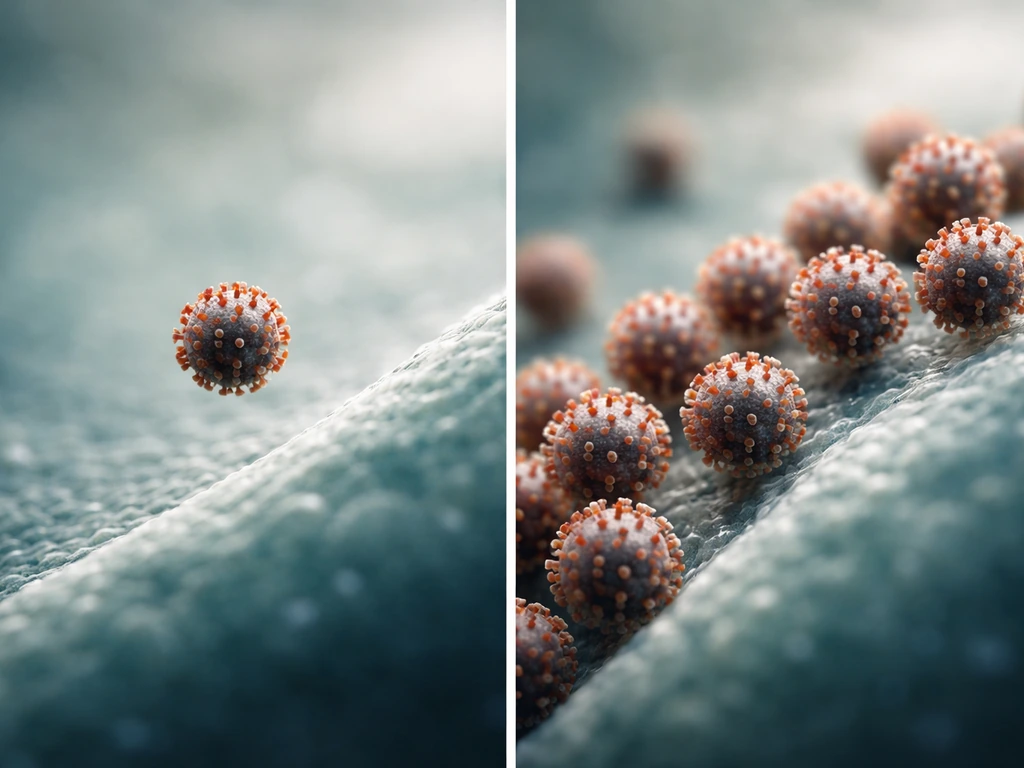
When a cell grows, it increases in size, synthesizes its own components, and eventually divides into two daughter cells through a process like mitosis. The cell is doing all of this work autonomously, using its own metabolism and internal machinery. Viruses do none of that. A single virus particle (called a virion) sitting on a surface is not growing, not eating, not repairing itself. It is essentially inert. Britannica describes viruses as entities that "should not even be considered organisms, in the strictest sense," precisely because they cannot carry out metabolic processes or reproduce without a host cell.
So what does change during a viral infection? Numbers change, not size. One virion enters a cell and, if conditions are right, that one infection event can produce hundreds to thousands of new virion copies that burst out and go on to infect other cells. That increase in particle count is what people loosely call viral "growth." The more precise word is replication. Think of it less like a seed growing into a plant and more like a photocopier: the original document does not change, but you end up with a lot more copies.
"Development" is similarly tricky to apply to viruses. In biology, development usually means a progression through distinct life stages, as in embryonic development or insect metamorphosis. Viruses do go through a sequence of distinct stages during replication (entry, genome copying, protein production, assembly, release), so in that narrow sense there is a kind of "development" happening. But it only makes sense to call it that inside a host cell. Outside one, nothing develops at all.
How viruses replicate: a step-by-step breakdown
The standard framework for viral replication, drawn from sources like OpenStax biology, breaks the cycle into six stages: attachment, penetration, uncoating, replication, assembly, and release. Here is what each step actually means.
Step 1: Attachment
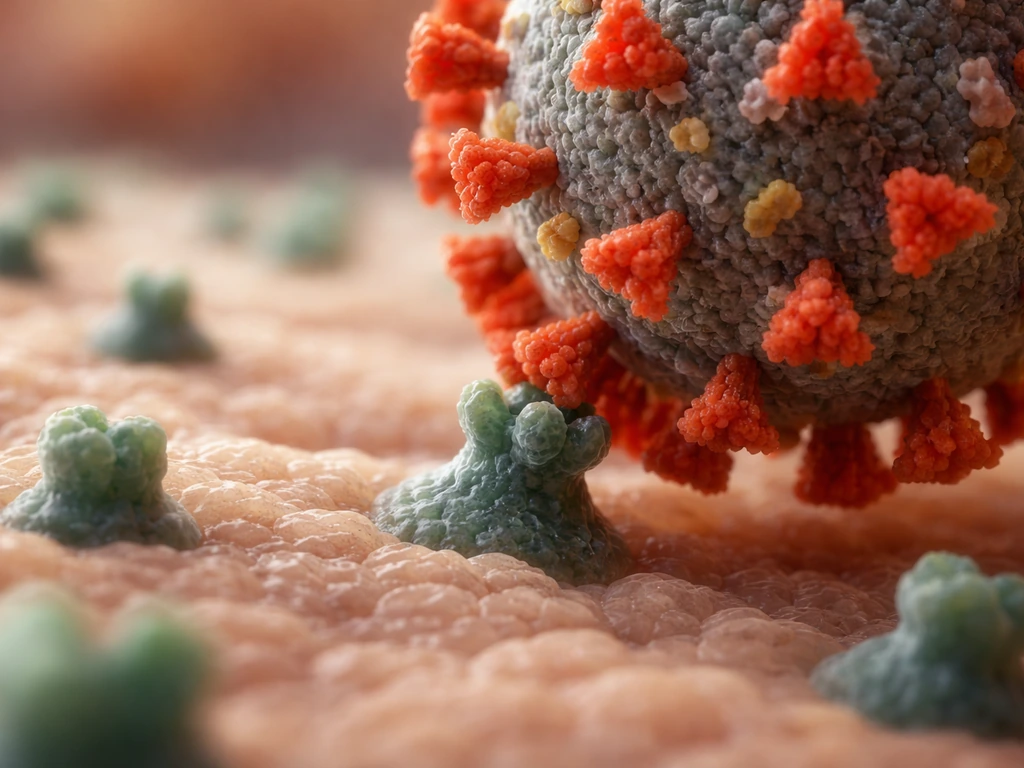
The virion docks onto the surface of a host cell by binding to a specific receptor. This is not random. A virus can only attach to cells that carry the matching receptor protein, which is why influenza infects respiratory epithelial cells while hepatitis B targets hepatocytes (liver cells). The virus is essentially using a lock-and-key fit to find the right door.
Step 2: Penetration (entry)
Once attached, the virus gets its genetic material into the cell. Some viruses fuse with the cell membrane. Others are engulfed by the cell through endocytosis. Either way, the goal is to get the viral genome inside.
Step 3: Uncoating
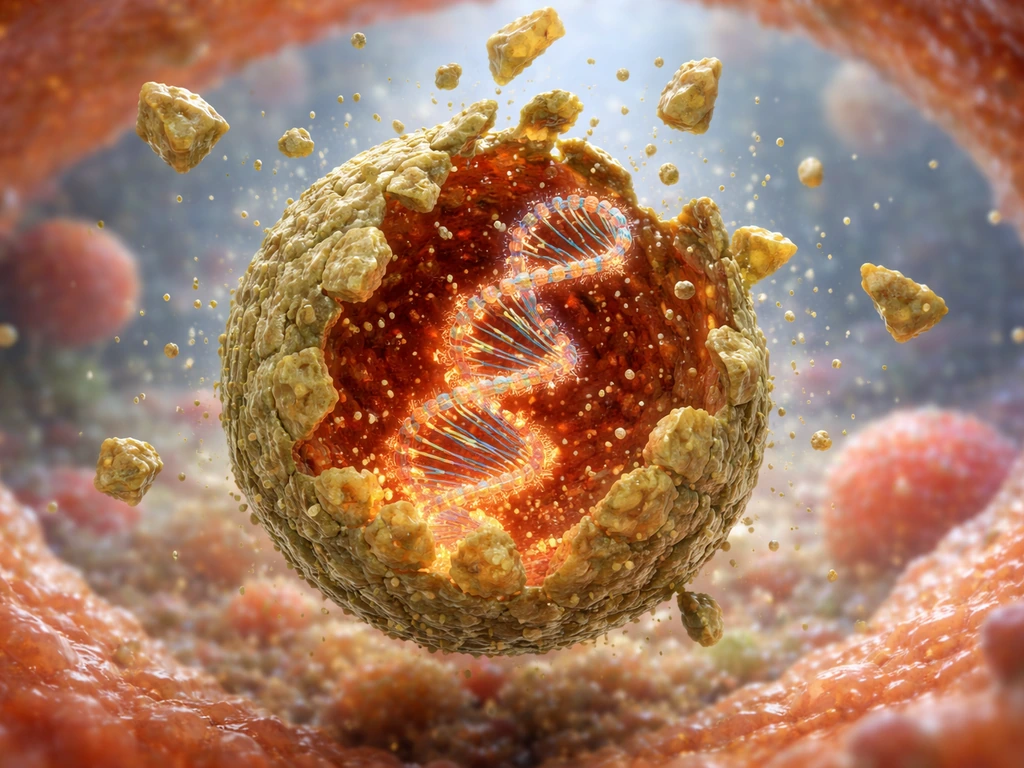
The viral capsid (its protein shell) is shed or broken down so the genome is exposed and available to be read. For influenza, a viral protein called M2 acts as an ion channel that acidifies the interior of the virus particle, triggering uncoating. This step is enzymatic and physicochemical, meaning it depends on specific conditions being just right. Interestingly, some viruses like reoviruses never fully uncoat; they carry out genome replication inside particles that still resemble the original virion.
Step 4: Replication (the eclipse period)
This is the heart of viral "development." The viral genome is read, viral messenger RNAs are transcribed and processed, viral proteins are translated, and the genome is copied many times over. During this period, called the eclipse phase, there are no complete new virions detectable in the cell. If you were watching under a microscope, it would look like nothing is happening. But inside, the cell's ribosomes and other machinery are being redirected to produce viral components. For coronaviruses like SARS-CoV-2, for example, the incoming genome is immediately translated into large polyproteins that are then cut into nonstructural proteins forming the replication and transcription complex.
One important detail: not all viruses use the same enzymes here. DNA viruses that replicate in the nucleus can often borrow the host cell's own DNA and RNA polymerases. RNA viruses face a bigger challenge because host cells do not have RNA-dependent RNA polymerases (enzymes that copy RNA from an RNA template) or reverse transcriptases. So RNA viruses and retroviruses have to bring their own. This is a fundamental part of why viruses are constrained in what they can do.
Step 5: Assembly
New genome copies and newly synthesized viral proteins are assembled into complete virion particles. This is where "maturation" happens, and it is the closest thing viruses have to biological development. Newly assembled particles are sometimes called immature virions and must undergo further processing (like protein cleavage) to become fully infectious. Think of it as the difference between a flat-pack box of parts and a fully assembled product.
Step 6: Release
Completed virions leave the host cell. Some viruses, like many bacteriophages, do this by lysing (bursting) the cell open. Others bud out through the cell membrane in a way that can be more gradual. Either way, this is the "burst" phase of what biologists call the one-step multiplication curve: a sudden jump in the number of infectious viral particles outside the cell.
Where do viruses replicate in the body and in nature?
Because attachment depends on receptor matching, each virus replicates in specific tissues and cell types. A few well-known examples:
- Influenza virus attaches to and replicates inside respiratory epithelial cells lining the trachea and bronchi. Viral replication destroys these cells, and it takes roughly 3 to 4 weeks for the epithelial lining to fully regenerate.
- Hepatitis B virus replicates specifically in hepatocytes, the main functional cells of the liver.
- Norovirus (the classic stomach bug) replicates predominantly in intestinal epithelial cells, particularly enteroendocrine cells in the small intestine.
- Herpes simplex virus (HSV) first replicates at oral or genital mucosal surfaces, then infects neuronal dendrites and can establish latency within sensory neurons, where the viral genome persists without active replication until reactivation.
Outside the body, viruses do not replicate at all. A virus particle sitting on a door handle, in a water droplet, or even in a lab dish without cells is completely inert. It cannot replicate in soil, water, or air. It can only survive long enough (depending on temperature, humidity, and whether its capsid or envelope stays intact) to reach a suitable host. This is a major distinction from bacteria or fungi, which can grow and multiply in many environments. If you are comparing viruses to the single-celled organisms covered elsewhere on this site, like Outside the body, viruses do not replicate at all. A virus particle sitting on a door handle, in a water droplet, or even in a lab dish without cells is completely inert. It cannot replicate in soil, water, or air. It can only survive long enough (depending on temperature, humidity, and whether its capsid or envelope stays intact) to reach a suitable host. This is a major distinction from bacteria or fungi, which can grow and multiply in many environments. If you are comparing viruses to the single-celled organisms covered elsewhere on this site, like amoeba or paramecia, the contrast is stark: those organisms grow and divide independently; viruses simply cannot. or paramecia, the contrast is stark: those organisms grow and divide independently; viruses simply cannot.
In aquatic environments, bacteriophages (viruses that infect bacteria) follow the same rule. They replicate inside bacterial host cells, not freely in the water. Environmental factors like temperature, salinity, and phosphorus availability can influence how readily a phage infects its bacterial host and whether it undergoes a lytic (burst-and-replicate) or lysogenic (dormant) cycle, but none of those factors allow replication without a living cell host.
What conditions allow viral replication to happen?
Three things need to line up for a virus to replicate successfully.
- A compatible host cell with the matching receptor. Without the right surface receptor, the virus cannot attach and the whole cycle stops before it starts.
- Access to the cell's internal machinery. The virus needs the host cell's ribosomes to translate its proteins, and in many cases its nuclear enzymes to copy its genome. A dead or severely damaged cell cannot supply this.
- Permissive environmental and cellular conditions. Temperature matters a lot. For example, research on fish viruses like infectious hematopoietic necrosis virus (IHNV) shows that water temperature directly affects replication efficiency. For human viruses, body temperature plays a similar role in whether a virus can replicate efficiently in a given tissue.
One concept worth knowing, especially for coursework, is multiplicity of infection (MOI). This is the ratio of virus particles to target cells in a given experiment or infection scenario. A higher MOI means more cells get infected simultaneously, which affects how fast the viral population grows at the population level, even though no individual virus is "growing" on its own.
Why viruses can't grow the way cells do
Even with a perfect host cell available, viral replication is fundamentally constrained in ways that cellular growth is not. Here is why unlimited viral growth is impossible.
| Constraint | What it means in practice |
|---|
| No autonomous metabolism | Viruses cannot generate energy, synthesize building blocks, or maintain homeostasis on their own. They depend entirely on the host cell for all of these functions. |
| Host cell destruction | Many viruses kill the cell they replicate in. Once the cell lyses or shuts down, that particular replication factory is gone. Influenza, for example, destroys respiratory epithelial cells as it replicates. |
| Genome size limits | Viral genomes are tightly constrained. Retroviruses like HIV have upper limits on how much RNA can be packaged; even small insertions near that limit can cripple replication. |
| Dependence on host enzymes (with gaps) | RNA viruses need RNA-dependent RNA polymerases that host cells do not have. If the virus cannot encode or deliver these enzymes itself, replication fails entirely. |
| Immune and tissue responses | The host immune system targets infected cells, and damaged tissues (like the respiratory epithelium) stop being permissive hosts as they regenerate and mount defenses. |
| Eclipse phase timing | The coordinated, staged nature of the replication cycle means there is a fixed lag before any new virions appear, and each infected cell produces a finite burst of particles rather than continuous growth. |
This is why viral infections tend to follow a characteristic curve: rapid expansion as the virus finds new permissive cells, then a plateau and decline as host defenses kick in and available host cells become scarce or resistant. It is a boom-and-bust pattern, not the steady growth you see in a dividing bacterial population or a growing multicellular organism.
Clearing up the common confusions
"Growing" vs. replicating
When someone says a virus "grows" in the body, they almost always mean its numbers are increasing, not that individual particles are getting larger. A virion is the same size when it exits a cell as when it entered. The confusion comes from using "growth" as a shorthand for population expansion, which is a reasonable everyday usage but technically inaccurate when applied to viruses.
"Developing" vs. maturing
Viruses do go through a kind of maturation during assembly. An immature virion is not yet infectious; it needs specific protein-cleavage steps to become a fully functional particle. That maturation process is sometimes loosely called "development," and it is not wrong to use the word in that limited context. Just be clear that it is not development in the same sense as embryonic development or the growth stages of a protist or bacterium.
Latency vs. active replication
Some viruses, like HSV, can persist in host tissues without actively replicating. This is called latency. During latency, the viral genome is present in cells but there are no new virions being produced and no detectable lytic transcripts. It is not a form of slow growth; it is more like a pause state. The virus can reactivate later and re-enter active replication. This distinction is important in coursework because latency is sometimes confused with slow or "quiet" replication.
The eclipse phase confusion
Students often get tripped up by the eclipse period because it looks like nothing is happening. In reality, this is when all the molecular work of replication is occurring: the genome is being copied, proteins are being made, components are being assembled. It is just that no complete, infectious virions exist yet. Then the burst phase hits and virion numbers spike suddenly. Understanding this staged process helps make sense of why symptoms of a viral infection can take time to appear even after exposure.
How to think about this in real life or coursework
The next time you see a question asking whether viruses grow and develop, run through this quick mental checklist: Do viruses increase in size? No. Do they divide like cells? No. Do they replicate and produce more copies of themselves? Yes, but only inside a living host cell with the right receptors and machinery. Does anything that counts as "development" happen? Only in the narrow sense of maturation during assembly, and only inside that host cell.
For practical purposes, whether you are studying for an exam, trying to understand how an infection progresses, or just satisfying curiosity, the most useful framing is this: viruses are replication machines, not growing organisms. Their "life cycle" is really a hijacking cycle. They bring instructions, the host cell does the work, and the result is more virions, not a bigger virus.
If you want to go deeper on how growth and replication differ across microbial life, it is worth comparing viral replication to how genuinely living single-celled organisms handle growth. Protists, for example, grow through cell division and have real autonomous metabolisms, which puts their growth biology in a completely different category from what viruses do. The contrast makes both topics clearer. how do diatoms grow