You cannot grow a fully functional, transplantable kidney from stem cells today, but you can grow surprisingly sophisticated kidney tissue in the lab. Scientists can now build kidney organoids (miniature kidney-like structures about 1 to 1.5 mm across) that contain real nephron cell types, form glomerulus-like and tubule-like structures, and even perform some basic kidney functions like protein transport and ion movement. That is genuinely remarkable. But a complete organ, with its million-plus nephrons, its intricate blood supply, its collecting ducts draining into a ureter, and its ability to filter 180 liters of fluid a day? That is still well beyond what any lab can produce. Here is exactly where things stand in 2026.
Can You Grow a Kidney From Stem Cells Today? What’s Possible

What 'growing a kidney' actually means right now
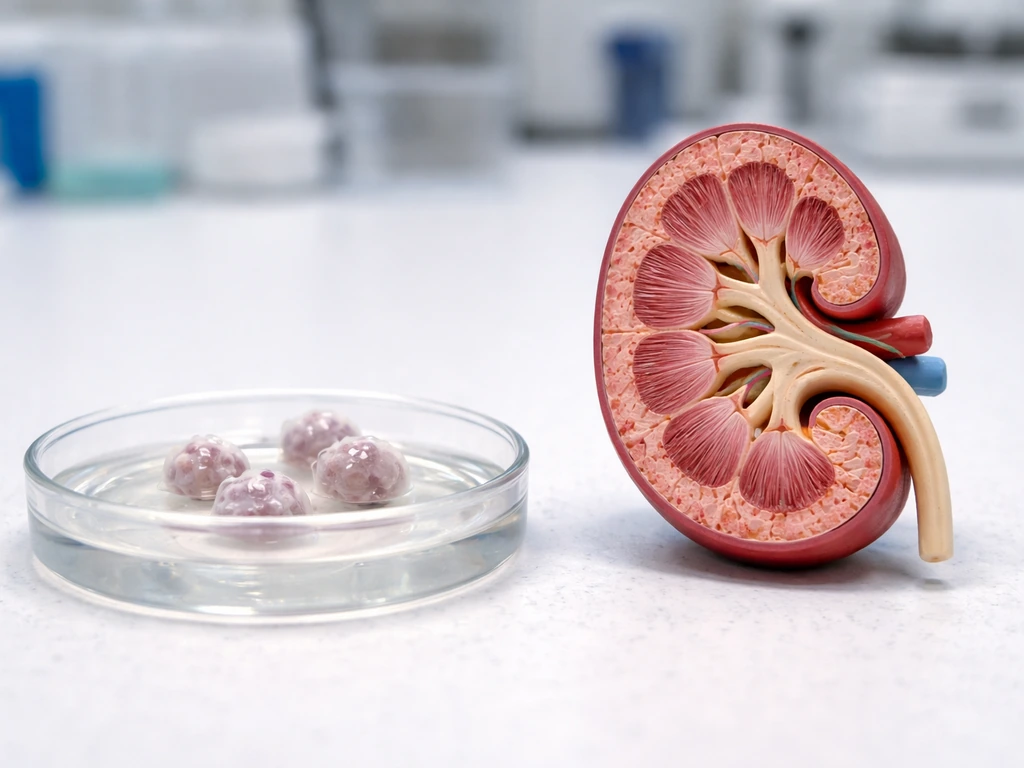
When people ask whether you can grow a kidney from stem cells, they are usually picturing a whole organ, something you could transplant into a patient with end-stage renal disease. That version does not exist yet. What researchers talk about instead falls into three categories, and it helps to be clear about the differences.
- Kidney organoids: self-organizing 3D clusters of stem-cell-derived kidney cells, typically a millimeter or two across, containing nephron segments like proximal tubules, distal tubules, and glomerulus-like structures. These are the main workhorse of kidney stem cell research right now.
- Collecting duct or ureteric bud organoids: a separate lineage of organoids that model the kidney's drainage system rather than the filtering nephrons. Researchers grow these independently and are actively working on fusing them with nephron organoids.
- Whole organ engineering: the long-term goal, combining all kidney compartments, full vascularization, and a ureter. This remains theoretical and preclinical in 2026.
Most practical progress is happening in the organoid space, and that is not a consolation prize. Organoids are already being used to model kidney diseases, test drugs, and study how the kidney develops. Understanding that distinction sets realistic expectations for everything else in this article.
Which stem cells are used, and how do you steer them toward kidney tissue
The main starting material for kidney organoids is human pluripotent stem cells, which includes both human embryonic stem cells (hESCs) and induced pluripotent stem cells (iPSCs). iPSCs are especially useful because they can be made from a patient's own skin or blood cells, reprogrammed back to a stem-like state, and then pushed toward kidney identity. That personalization matters enormously for disease modeling and, eventually, for transplant compatibility.
Adult kidney stem cells and progenitor populations also exist in the kidney itself, but they are more limited in what they can become. For building complex kidney tissue from scratch, pluripotent stem cells are the real tool of choice.
Directing pluripotent cells toward a kidney fate is not simple. The kidney develops from a region of the early embryo called the intermediate mesoderm, so researchers have to walk cells through the same developmental checkpoints the embryo uses. The general signaling logic goes like this: you expose cells to combinations of molecules that push them from a naive pluripotent state through a posterior primitive streak stage, then into intermediate mesoderm, and finally into nephron progenitor populations. Key signals involved include BMP (bone morphogenetic protein), FGF (fibroblast growth factor), retinoic acid, and Wnt pathway activators, applied in precise sequences and concentrations. For ureteric bud or collecting duct organoids, the protocol branches differently, using FGF2 and retinoic acid alongside inhibitors of TGFβ and BMP signaling to steer cells toward that lineage instead.
How kidney development informs the way organoids are built
Think of organoid construction as reverse-engineering embryology. During normal kidney development, two populations of cells talk to each other constantly: the metanephric mesenchyme (which generates the filtering nephrons) and the ureteric bud (which branches repeatedly to form the collecting ducts and ultimately the ureter). Their back-and-forth molecular conversation is what drives the kidney's branching architecture and its characteristic arrangement of around a million nephrons in a human adult kidney.
Organoid protocols try to recapitulate those conversations in a dish. The landmark 2015 work by Takasato and colleagues showed that human pluripotent stem cells could be coaxed into kidney organoids containing multiple nephron cell types and structures that resembled glomeruli and tubules, essentially modeling a slice of nephrogenesis in 3D. That paper established the template that most research groups have been building on and refining ever since.
The staged signaling approach matters because kidney cells are not just 'kidney cells.' A proximal tubule cell, a podocyte in a glomerulus, a collecting duct principal cell, and an intercalated cell are all wildly different in function and gene expression. Getting the right mix in the right spatial arrangement requires hitting each differentiation checkpoint correctly, which is why protocols are measured in days and involve carefully timed additions of growth factors and small molecules.
What scientists can actually build today
Current kidney organoids are genuinely functional in several measurable ways, which is worth appreciating. A 2025 Nature Communications study showed that proximal tubule-like cells in organoids can take up albumin (a protein the kidney normally reabsorbs), demonstrating real transporter activity using fluorescently labeled albumin and LRP2 antibody readouts. Collecting duct organoids derived from pluripotent stem cells can produce AQP2-positive principal cells by around day 18 of differentiation, and some show amiloride-sensitive vectorial sodium transport, meaning they are moving ions the way real collecting duct cells do. Patch-clamp measurements have even confirmed functional BKCa ion channels in iPSC-derived kidney organoids.
Transplanting organoids under the kidney capsule of immunodeficient mice has pushed maturation further. After subcapsular transplantation, organoids develop CD31-positive glomerular endothelial structures and PDGFR-β-positive pericytes, meaning the tissue starts to recruit and organize a vascular supply in a living environment. That is a big deal because vascularization in a dish is one of the hardest problems to solve.
Researchers have also recently reported fusing distal nephron segments to ureteric bud organoids to begin integrating the nephron and collecting system sides of kidney biology into a single construct. That kind of assembly work is exactly what would need to scale up for anything approaching a whole organ.
| What has been achieved | Current status (2026) |
|---|---|
| Nephron organoids with glomeruli and tubules | Routine in multiple labs, well-established protocols |
| Collecting duct organoids with AQP2+ principal cells | Achievable by ~day 18 with directed differentiation |
| Proximal tubule albumin uptake (functional transport) | Demonstrated in 2025 with quantitative assays |
| Vectorial ion transport in collecting duct lineage | Demonstrated (amiloride-sensitive sodium transport) |
| Patch-clamp confirmed ion channel function | Demonstrated in iPSC-derived organoids |
| Vascularization in vivo (subcapsular transplant) | Achieved in mouse models, not yet in clinical settings |
| Nephron-to-collecting duct fusion in one construct | Early-stage, reported in 2025 |
| Transplantable whole kidney from stem cells | Not achieved, not in clinical trials |
Why a full kidney is still out of reach
The gap between a 1.5 mm organoid and a full kidney is not just a size problem. It is an architecture problem, a vascularization problem, a maturation problem, and a connectivity problem all stacked on top of each other.
Architecture and nephron number
A human kidney contains roughly 800,000 to 1.2 million nephrons, each one a precisely organized tube that filters blood, reabsorbs what the body needs, and delivers waste to the collecting system. Every nephron has to be wired up correctly in 3D space. Current organoids contain nephron-like units but in far smaller numbers, less organized spatial arrangement, and without the radial architecture of a real kidney. Nobody yet knows how to template that full 3D structure in the lab.
Vascularization and oxygen supply
This is arguably the single biggest wall. A kidney is one of the most blood-rich organs in the body, receiving about 20 to 25 percent of cardiac output. Every nephron needs intimate contact with a capillary bed (the glomerular capillaries do the actual filtration). Growing tissue thicker than about 1.5 mm in a dish creates oxygen and nutrient gradients that kill cells in the center. Even the most sophisticated vascularization engineering approaches, including genetically engineering endothelial niches inside organoids, have not solved the problem at scale. In mice, organoids can recruit blood vessels after transplantation, but that is far from a kidney-sized vascular tree.
Collecting system connectivity
Filtering is only half the job. The kidney also has to drain. Filtered waste has to flow from nephron tubules into collecting ducts, down the renal pelvis, and out through the ureter to the bladder. In most current organoid systems, the nephron progenitor lineage and the ureteric bud/collecting duct lineage are grown separately and have not been fully integrated. Transplanting a kidney-like tissue without a connected urinary exit tract would just produce a structure that fills with fluid and fails. The 2025 fusion work is a meaningful step, but it is early.
Maturation
Even the best kidney organoids today are developmentally fetal-like. Adult kidney cells are specialized in ways that take months of development and postnatal maturation to achieve. Organoid cells express markers and perform functions reminiscent of fetal kidneys, not adult ones. That matters enormously for filtration capacity, drug handling, and long-term stability after transplantation.
The practical barriers to scaling up
Even setting aside the biology, actually manufacturing kidney tissue at clinical scale introduces a different set of problems. Growing organoids reproducibly across labs is already a challenge. Protocols that work well in one research group can fail in another because of subtle differences in cell lines, batch variation in growth factors, or culture conditions. The NIH recognized this seriously enough that in 2025 it established the country's first dedicated organoid development center specifically focused on standardization and reproducibility across labs, with the goal of creating organoid models that regulators will accept.
Manufacturing for transplant would also require moving from small research batches to Good Manufacturing Practice (GMP) conditions, using tightly controlled, well-characterized reagents. The FDA issued guidance in April 2024 specifically addressing the use of human and animal-derived materials in cell and gene therapy manufacturing, which gives a sense of how seriously regulators are watching this space and how many production variables need to be locked down before any clinical use.
Integration with the recipient's body adds another layer. A transplanted kidney-like construct would need to connect to blood vessels, drain through a ureter, and avoid triggering immune rejection, all simultaneously. Even in animal models, achieving stable, long-term vascularized integration of organoid-derived tissue has not been demonstrated at the scale needed for a functioning kidney.
Safety, ethics, and what to realistically expect next
Safety is not a minor footnote here. When you use iPSCs (reprogrammed stem cells) to grow tissue for potential transplant, there is a real risk that not all cells fully committed to the kidney fate. Residual pluripotent cells in a transplanted construct could form tumors. Research testing kidney organoids for tumor-forming potential has found that while these organoids do not form teratomas (the classic pluripotent stem cell tumor), they can form other tumor types, which means rigorous safety screening before any clinical use is non-negotiable.
The ethics of this work are worth thinking about clearly too. iPSC-derived kidney organoids sidestep many of the ethical concerns around embryonic stem cells because they come from adult donors. But as organoids get more complex and more physiologically realistic, new questions arise about how to classify them, especially in the context of chimeric research (growing human organoids in animal hosts for maturation). Regulatory frameworks are still catching up to the science.
So what should you actually watch for in the near term? A few things are genuinely close to moving forward. Better vascularization strategies, including bioengineered scaffolds and microfluidic chips that mimic blood flow, are advancing quickly. The nephron-to-collecting duct fusion work could mature into a more complete organoid platform within a few years. Subcapsular transplantation studies in animals will likely generate more functional maturation data. And standardization efforts from NIH and regulatory bodies will make the path to clinical trials clearer, even if those trials are still years away.
It is also worth noting that the same fundamental biology driving kidney organoid research applies to other organs. The stem cell differentiation logic, the vascularization barriers, the maturation gaps, and the safety questions are shared challenges across efforts to grow livers, hearts, pancreatic tissue, and skin from stem cells. The same stem-cell technologies being used to build kidney organoids also underpin efforts to grow livers from stem cells. Progress in any one of these areas tends to accelerate the others, so kidney organoid research does not happen in isolation.
The honest summary: growing a kidney from stem cells is not science fiction, but it is not science fact yet either. So, can you grow a heart from stem cells? You can apply the same stem-cell organoid approach to pancreatic tissue, but growing a fully functional pancreas from stem cells is still far from clinical reality can you grow a pancreas from stem cells. Not yet, but researchers are actively working on heart tissue models and maturation strategies. What exists in 2026 is sophisticated kidney tissue that can do real kidney-like things at small scale, inside a dish or inside an animal. The path to a transplantable organ is real and actively being built, but it will require solving vascularization, architecture, maturation, and manufacturing problems that are each significant on their own. If you are following this field, the organoid work happening right now is the foundation everything else will be built on.
FAQ
Can you grow a kidney from stem cells for transplant today?
No. The lab-produced kidney-like tissue is not a complete, scalable organ with adult-level filtration capacity, integrated vascular networks, and a functional urinary drainage connection to a ureter and bladder. Most work remains at the organoid level (millimeter scale) or early tissue constructs in animals.
What’s the difference between “kidney organoids” and a “kidney organ”?
Organoids are simplified, self-organized pieces that contain kidney-relevant cell types and some function, but they do not replicate the full organ’s organized 3D architecture, nephron count, and integrated blood and urine pathways. A transplantable kidney also needs long-term stability and controlled maturation, not just short-term function.
Can iPSCs made from my own cells reduce rejection risk if a kidney tissue reached transplant readiness?
They could help with immune compatibility because iPSCs can be patient-matched, but rejection risk is not eliminated. The final transplant still depends on how the tissue is processed, whether any non-kidney cells remain, and how the construct integrates with host vasculature and immune surveillance.
Why do most kidney organoids stall at a fetal-like stage?
Kidney maturity depends on time, signals, and physical context that are difficult to replicate in a dish. Adult specialization requires prolonged developmental cues and maturation after vascular and structural organization are established, which is why organoid function may look “kidney-like” but not fully adult.
How big can kidney tissue grow in culture before cells die?
A common practical limit is around the millimeter range (often described as roughly 1.5 mm), because oxygen and nutrient gradients become damaging. That is why increasing thickness requires vascular-like delivery strategies, not only more growth factors.
Do kidney organoids actually filter blood like real nephrons?
They can show specific kidney behaviors, like transporter activity and ion movement, and may form glomerulus-like structures, but they do not yet replicate the complete filtration unit performance at organ scale. The key missing piece is robust, correctly perfused capillary networks that support sustained filtration.
Can organoids be connected to urine outflow in a way that prevents fluid buildup?
Current systems often grow nephron-like tissue and collecting-duct lineage separately, so true, reliable urine drainage pathways into a ureter-like exit are not consistently achieved. Early fusion approaches are promising, but a mature, fully connected urinary tract remains a major hurdle.
What are the biggest technical obstacles beyond making the right cell types?
Four recurring bottlenecks are vascularization at kidney scale, correct 3D nephron architecture and spatial wiring, maturation to adult-like function over long timelines, and integration with blood and urine pathways after implantation. Each one interacts with the others, so improving one often does not automatically solve the rest.
Is tumor risk a concern for iPSC-derived kidney tissue?
Yes. If any residual pluripotent cells remain, they could form tumors after implantation. Even when classic teratomas are not observed, other tumor-like risks can exist, so stringent purification and testing for tumor-forming potential are essential.
Why do organoid results sometimes differ between labs?
Subtle variations in starting cell lines, batch differences in reagents, and timing of growth-factor dosing can shift differentiation trajectories. That is why standardization initiatives are focusing on reproducible protocols, defined inputs, and consistent quality control measurements.
What would “GMP manufacturing” change compared with research lab culture?
GMP-grade production requires tightly controlled, well-characterized reagents and procedures, documentation of every critical variable, and release testing for identity, purity, potency, and safety. Scale-up also changes logistics, timing, and allowable handling steps compared with academic organoid workflows.
How close is research to integrating nephron and collecting system lineages?
There are early reports of fusing distal nephron segments with collecting-duct organoids to make more integrated constructs. While that is a meaningful step toward coordinated urine handling, it is still early relative to building a whole-organ system with reliable drainage.
If kidney organoids can’t be transplanted yet, what are they useful for right now?
They are already valuable for modeling kidney disease processes, testing drug responses, and studying developmental biology and signaling pathways. This can accelerate therapy discovery even before a transplantable kidney exists.
Could progress in kidney organoids help other organs too?
Yes. Many constraints are shared across organoid fields, including directing correct lineage identity, overcoming oxygen and nutrient limits, achieving vascularization, ensuring maturation, and managing safety. Improvements in any one organ platform often carry over to others.
Can You Grow a Pancreas From Stem Cells? What’s Real
Explains whether stem cells can make pancreatic tissue, organoids, and beta cells, and what blocks a full transplant pan


